How common is Plantar Fasciitis?
Plantar fasciitis, plantar faciopathy or plantar heel pain (all terminology gets used interchangeable despite different definitions existing) affects 15% of all running injuries in the foot.
It’s estimated that one in ten people will experience foot pain or plantar fasciitis in their lifetime. The reason is the foot absorbs forces of three times the body weight when you’re running. So the plantar fascia, (plantar just simply means the sole, the bottom of your foot), is a thick elastic tissue that stretches from your heel at the base of your foot and inserts into each of the five metatarsal bones in your foot. It’s role is to stabilise the inner forces that peak during push off. This can be as much as seven times your body weight. So simply put it takes a lot of load during running or walking and is a very strong structure.
Plantar fasciitis is a self limiting condition and does get better over time. So the good news is if you do absolutely nothing this condition and you just leave it on its own, it will recover in the majority of cases. The downside, this process can take up to a year to get better without doing any rehab or treatment. It’s common for this condition to develop at two stages in life around your 40’s and 60’s.
Some of the symptoms of plantar fasciitis include a sharp stabbing pain or deep ache in the arch of your foot or bottom of your heel. Some people describe it as “like walking on glass” when they first wake up in morning. You get stiffness and pain first thing in the morning so a lot of people have to wear a trainers as soon as they get out of bed, they have to put their shoes on because it’s really, really painful. It worsens throughout the day as the body fatigues, and the pain worsens when they climb stairs. It’s a nagging injury, so running through it can delay healing, so if you don’t address it right away it can become chronic and it can niggle away and last months. It’s a condition which is frustrating and annoying.
Some of the causes of plantar fasciitis include over-training. Too much, too soon, particularly in those who are just starting running or returning from another injury. Some vigorous hill runs or speed work can cause it due to the higher forces and foot striking. Neglecting to stretch the calve muscles is another contributing factor. Tight calves can be one the main risk factors for this condition. The calf muscles, if their range becomes shorter, contribute to this condition as it attaches onto your Achilles tendon which runs into your plantar fascia. As a result this then increases the load onto that structure, potentially causing a problem.
Wearing unsupportive shoes, can also contribute. The classic example is when you go on holiday and you think, “Okay, I’m going to wear my flip flops for a week or so.” And then you’ve not got that support in your arch and after a couple of days on holiday, you’re thinking, “Oh my goodness, my heel’s really, really sore.”
Simply that’s because you’ve not got that support, and that tends to be an issue.
Starting a running program too aggressively or lack of foot strength, or the too much, too soon approach can all initiate this condition. You think, “Okay, I want to push myself.” You might do too much, too soon, then you start to get a little bit of pain and a lot of people think, “Right, okay, it’s just a little bit of pain, I’ll push through.” And then it gets to the point when you can’t run anymore, and then you think “I’ll keep going, I’ll just keep going.” But in actual fact, the more you keep going, it becomes a chronic issue and the more difficult it is to go away. There can also be biomechanical factors, so if you’ve got a high arch, or low arch which is normal, but in some people can contribute to this condition.
The treatment includes mobilising tight structures and fascia, and strengthening your foot muscles. So there’s new research suggesting a strengthening and phased loading protocol, which includes calf raises with the addition of your big toe on top of a rolled towel. That’s the most effective evidence based treatment at the moment for the rehab for plantar fasciitis. Manual stretching your foot by pulling your toe back lengthening that plantar fascia can feel nice but only gives short term relief, that’s because the facia is strong and can’t be stretched. However, this ensures the plantar fascia has good mobility as you are not going to change your flexibility given how strong a structure it is.
So physiotherapy to mobilise and release tight fascia in the foot is used in those with more acute presentation. The different techniques you can use include soft tissue techniques, massage, different active-release techniques that can definitely be beneficial for releasing the bottom of the foot and early strengthening, so it’s not just looking at the foot itself, although the pain is localised to the foot, this includes the calf, the hamstring, or the gluteal muscles.
Cross training with water, running, swimming, elliptical and cycling, are good solutions when you find running very painful. It might be the case that we can still perform some training but it may be that we need to alter your training methods, so that we’re not loading the foot just as much as before. For example running in the water, so that the load through the foot is not as high, or cycling, this approach may allow us to run one day and the next day we might change so it’s a different method of getting fit but also not loading the foot. We may also perform gait analysis as part of your assessment, which we use in our clinics, to see how your foot performs when it is in contact with the ground while running and walking. This allows us to see who benefits from a custom made orthotic to reduce pain levels and optimise the performance of the foot.
Prevention is one of the main things we look at including running on a variety of surfaces. So if you’re constantly running on a hard surface and it’s causing you pain then we need to look at changing the surface, softer surfaces, dirt paths, grass or trails rather than the concrete, and then just changing so it’s not always on the same surface. This exposes the foot to different environments and helps its recovery. It also allows us to keep you running as we rehab the injury.
Your running shoes may also play a role. Making sure they fit properly and they’re not overly worn. If you’ve had them for years and they’ve lost their shock absorption and they don’t provide adequate support then this may be contributing to your problem.
A personalised progressive training program is essential.
So is it right for your ability? Your stage in healing? And aligned with your goals? You need to make sure that you’re not doing too much too soon, but also loading it enough to help it recover. Rest is not the answer here. We would look at your previous exercise levels, if you’ve not really been that active before, or if you’re doing high levels for example marathon distance or above then you’re at higher risk of getting an injury, so you need to make sure that it’s structured to your exercise levels.
Foot strengthening exercises should be included in your program but they are not the silver bullet. The body works as a chain and different parts of the chain can contribute to the problem. This might include addressing tight hip flexors or core strength, things that you might not think about because the pain is located in the foot. You think, “Okay, I need to work on just the foot.” But actually you need to work up the chain, as this can be contributing to why you’re getting the pain in the first place. For example research has suggested that lower back pain or history of injury in your lower back has correlation with plantar fasciitis.
Our 5 Simple Steps to Help Your Plantar Fasciitis
Step 1: Get an accurate assessment and diagnosis
Get an expert option and personalised treatment plan based on your injury, stage of healing, biomechanics and training level. We can’t treat everyone with the same exercises or loading protocol. Human bodies are far more complex and don’t all respond the same way. This is exactly why Dr Google simply doesn’t work for plantar fasciitis or any other condition for that matter. We need to be able to filter out the relevant information and make a plan specifically for you to maximise your recovery. We will include a gait analysis as part of your assessment, usually in your 2nd appointment. This may also include a recommendation for custom made orthotics. These are not suitable for everyone but for the right patient they can make a huge difference.
For more information about this click this link.
Step 2: Ankle and foot mobility
Physiotherapy or a podiatrist can help identify and treat with hands on manual techniques to help accelerate your recovery. This all comes after the assessment as we can determine where the restrictions possible exist in the ankle, Midfoot or forefoot. From there we can begin to give you some relief and improve how the pain behaves.
For more information on foot and ankle problems check out this page
Step 3: Strengthening
Managing load is key. We can help you to identify contributing factors and discuss what you can do. We don’t like telling people to completely stop exercising – it’s about finding a balance and some alternatives to the pain provoking activities. Finding this balance allows the repair process to be most successful.
Your rehabilitation plan will include exercise to improve ankle and foot mobility, foot strength and calf and achilles tendon strength. Exercise is linked with better outcomes in the short and long term.
Step 4: Shockwave therapy
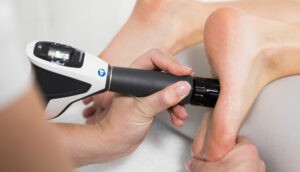
Shockwave is a safe and effective non invasive treatment which is evidence based and perfect for people with plantar fasciitis who want to get better faster. It is applied through a handheld device, which can either be focused specifically to one point or generally depending on the desired effect. The “shockwaves” or pulses produced by this device create movement within the cells of the targeted structures as they pass through them, encouraging an increase in cell activity. Within this increase, the cells request a higher demand for blood supply, helping with recovery. They also release additional beneficial chemicals which aid the recovery process and offer pain moderation.
So in summary shockwave therapy helps with 3 key responses to plantar fascia pain:
1. Reduces pain response
2. Stimulates the repair and promotes tissue healing response
3. Controls the inflammatory response to allow for a faster recovery
For more information click here.
Step 5: Do the work and be patient
Follow this process and be consistent. Research has shown that it can take 12-16 weeks to resolve plantar fascia pain and that is consistent with my clinical experience in physiotherapy. This is clearly a long time when your in discomfort everyday, but it certainly much more preferable than 1-2 years if you leave to nature alone. So don’t expect a quick fix, but you can expect to stop worrying about making it worse, avoid surgery and make a full recovery if you follow the plan and stick to it. We will help guide and support you all the way.
Bonus Tip: Nutrition for plantar fascia pain
Give the body the nutrition and conditions it needs to repair. For instance the plantar fascia is made from collagen which is formed from protein. If you have an inflammatory reaction, then an anti inflammatory diet can also help. Additional Vitamin D3 is crucial for health of tissues, and 50% of the population suffer from Vit D deficiency. This can really help your symptoms without relying on pain relief or pharmaceutical medications.
Are you ready to get better?
If so call us on 0333 3010205 and arrange a free 15minute consultation to get started and make sure it is the correct next step for your problem.


0 Comments